Understanding Occipital Lobe Seizures: The Story of Olivia
Occipital lobe seizures are focal seizures that begin in the back of the brain, in the region responsible for vision. Because they often produce flashing lights, visual distortions, brief blindness, or unusual eye movements, they are frequently mistaken for migraines or dismissed as simple visual disturbances. In this post, we will explore what occipital lobe seizures are, how these seizures present in both children and adults, and how they are diagnosed and treated. Through the story of Olivia, you will see how subtle visual symptoms can unfold into a clear neurological pattern and why careful attention to detail can lead to the right diagnosis and treatment plan.
Dr. Clotilda Chinyanya
2/6/20265 min read


Olivia’s Story
Olivia first noticed it during an evening walk.
The sun had already dipped below the horizon, and streetlights were flickering on one by one. As she crossed the street, a burst of color flashed in the right side of her vision. At first, she thought it was a reflection from a passing car. But the lights did not behave like reflections. They formed bright, circular shapes, shimmering in reds and greens, pulsing like small fireworks inside her field of view.
She stopped walking.
The shapes clustered in the same corner of her sight, never moving across the entire scene. They lasted less than a minute. When they faded, she felt slightly disoriented but fully aware. A dull headache crept in afterward.
She blamed stress.
A week later, it happened again while she was scrolling through her phone at night. This time, the lights were followed by a moment when everything in that same part of her vision went dark. It was not that she closed her eyes. It was as though a curtain dropped over part of the world.
Her eyes fluttered rapidly without her control. Her head turned slightly to one side. She could hear her husband asking if she was alright. She could respond. She just could not stop her eyes from pulling to the right.
The episode ended quickly. The headache returned, stronger this time, with nausea trailing behind it.
Her primary care provider initially suspected migraine with aura. That made sense. Visual changes and headache often go together. But something did not fully match. Olivia’s visual events were very brief. They were stereotyped, meaning they occurred the same way each time.
And sometimes, they happened without a headache at all.
When she saw a neurologist, she was asked a simple but powerful question.
How long do the lights last.
Olivia thought carefully.
Less than two minutes.
That detail changed everything.
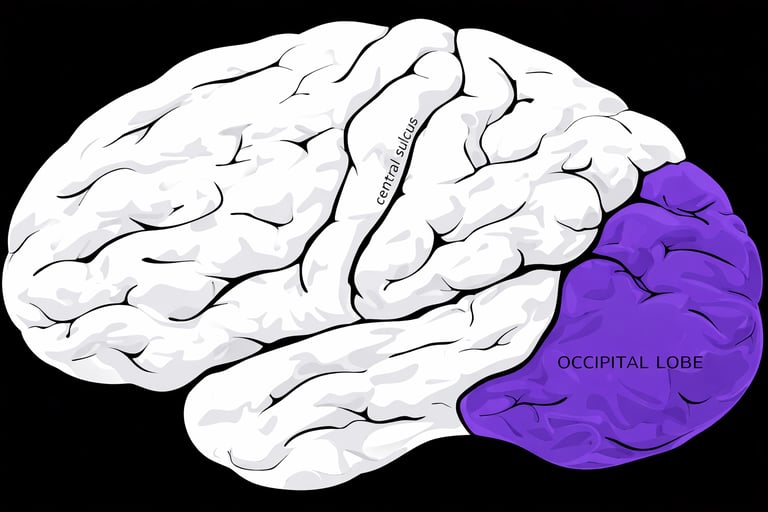
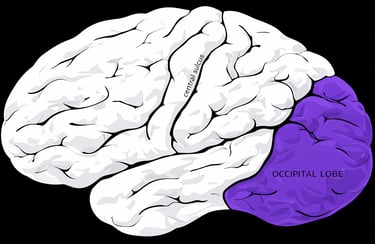
Where Is the Occipital Lobe Located and What Does It Do
The occipital lobe sits at the very back of the brain, just above the base of the skull. See image below:
The occipital lobe is the primary visual processing center. When light enters your eyes, signals travel through the optic pathways to the occipital lobe, where they are interpreted into color, shape, motion, depth, and recognizable objects and faces (1,4). In simple terms, the occipital lobe allows you to see and understand what you are seeing. It transforms raw visual input into meaningful perception. When a seizure begins in this region, symptoms usually affect vision first.
What Is an Occipital Lobe Seizure
Occipital lobe seizures are focal seizures that originate in the visual cortex at the back of the brain (1). They are considered rare compared with temporal lobe epilepsy and account for a small percentage of focal epilepsies. Because the occipital lobe is specialized for visual processing, these seizures often produce visual symptoms that can be subjective and difficult to describe, especially in children (1).
Types of Occipital Lobe Seizures
Primary Visual Cortex
Seizures arising from the primary visual cortex cause simple visual symptoms such as flashing lights or colored shapes, or negative changes like partial vision loss or brief blindness. Vision may rarely go completely dark or bright in both eyes. The disturbance appears in the visual field opposite the side of seizure onset, and the person may look toward that area. In children, drawing what they see can help clarify symptoms. Episodes are typically brief, often under two minutes, helping distinguish them from longer lasting migraine aura (1).
Extra Striate Cortex
Seizures in this region can produce detailed visual hallucinations, including images of people, animals, or entire scenes. These events are classified as focal cognitive seizures (1).
Parieto-Occipital Junction
Seizures in this region may involve rapid eye movements called epileptic nystagmus. The eyes may pull to one side, sometimes with head turning. Awareness is often preserved (1).
Inferior to the calcarine fissure
Seizures that begin in this region often spread to the temporal lobe, leading to focal seizures with impaired awareness (1).
Superior to the calcarine fissure
Seizures that start in this area may extend to the parietal lobe, fronto parietal operculum, or frontal lobes. If the spread to the frontal regions is rapid, it can result in focal atonic motor seizures (1,2).
This explains why some people can have sleep related hypermotor behavior even when the seizure originates in the occipital lobe (2).
Common Symptoms
Occipital lobe seizures can include:
• Visual hallucinations such as flashing lights or colors
• Partial or complete visual loss
• Eye blinking, forced eye closure, or eye deviation
• Nystagmus
• Nausea and vomiting in certain childhood forms
• Headache after the seizure
• Light triggered seizures in photosensitive forms
Because headache and nausea may follow, these seizures are frequently mistaken for migraines (4).
Childhood Forms of Occipital Epilepsy
There are recognized childhood syndromes involving the occipital lobe.
· Panayiotopoulos syndrome typically appears between ages three and six and often includes nausea and vomiting as prominent features. Most children have relatively few seizures and normal development (4).
· Idiopathic childhood occipital epilepsy may present later in childhood and often includes visual symptoms. In many cases, symptoms improve or resolve within several years (4).
· Photosensitive occipital lobe epilepsy involves seizures triggered by flickering lights such as video games or television (4).
These childhood forms generally have a more favorable prognosis compared with structural occipital epilepsy in adults.
Causes
Occipital lobe seizures may be caused by:
• Structural abnormalities such as tumors, vascular malformations, or scarring
• Developmental or genetic factors in childhood syndromes
• Trauma, stroke, infection, or metabolic disorders
• Photosensitivity
In some individuals, imaging reveals no clear structural cause.
Diagnosis
Diagnosis relies on careful history, EEG, and brain imaging.
EEG may show occipital spikes or posterior abnormalities (1). MRI helps identify structural causes. Because visual symptoms are subjective, asking patients to describe or even draw what they see can be helpful, especially in children (1).
Distinguishing occipital seizures from migraine is critical. Key clues include:
• Short duration, often under two minutes
• Stereotyped pattern
• Eye deviation or motor features
• Occurrence without headache
Treatment
· Treatment typically begins with anti-seizure medications. Many individuals achieve good seizure control with medication alone (4).
· If seizures are drug resistant and a structural lesion is identified, surgical intervention may be considered. In select cases, neuromodulation devices may be used, particularly in refractory epilepsy confirmed through specialized monitoring (2).
· Avoiding known triggers, such as flickering lights in photosensitive forms, can also reduce seizure frequency.
Olivia’s Outcome
Olivia’s EEG showed occipital spikes. Her MRI was normal.
· She was started on anti-seizure medication, and her episodes decreased significantly. The brief flashes that once frightened her became rare.
· She also made small adjustments. She reduced nighttime screen exposure, improved sleep consistency, and tracked any recurring patterns.
· Most importantly, she understood what was happening. Her brain was not failing her. It was misfiring briefly in the visual cortex. With treatment and monitoring, she regained confidence in her daily life.
Final Thoughts
Occipital lobe seizures can be subtle, brief, and easily mistaken for migraines or visual disturbances. Yet their pattern, duration, and associated eye movements tell a different story. The occipital lobe, located at the back of the brain, is responsible for interpreting visual information. When seizures begin there, vision becomes the language of the brain’s electrical disruption.
If you experience brief, repetitive visual phenomena that are difficult to explain, especially if they last less than two minutes or involve eye pulling or temporary visual loss, seek neurological evaluation. Careful history and proper testing can make the difference between years of confusion and effective treatment.
References
International League Against Epilepsy EpilepsyDiagnosis.org Occipital Lobe Seizure Overview
https://www.epilepsydiagnosis.org/seizure/occipital-overview.htmlSleep Related Hypermotor Epilepsy Originating from the Occipital Lobe Springer 2024
https://link.springer.com/article/10.1007/s10143-024-02772-8Occipital Lobe Epilepsy Review Wiley Epilepsy and Behavior Reports
https://onlinelibrary.wiley.com/doi/epdf/10.1002/epd2.20285Medical News Today What to Know About Occipital Lobe Epilepsy
https://www.medicalnewstoday.com/articles/occipital-lobe-epilepsy
Choose Knowledge: